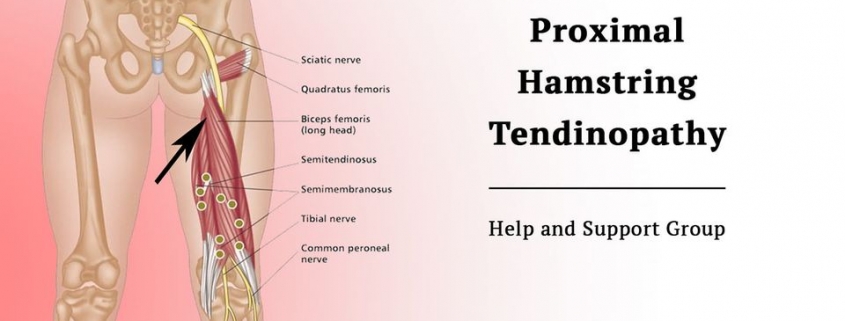
Proximal Hamstring Tendinopathy Recovery Stories
Corina Barbaza Weber’s Recovery
After fighting for almost one year PHT, just completed now a pain free, injury free half marathon in 1h37min, beating my 2016 PB. For everyone out there who is exasperated of not being able to sit without pain, let alone bend forward or run, I tell you: don’t lose hope. Stay focused, wrap yourselves in KT tape and don’t miss your boring Physio, massages and gym sessions with eccentric hamstring exercise and planks. God bless you and give you the strength to fight until you’ll get healed!

Mary Bourne-Marth’s Recovery
After 2 years of fighting, PT + dry needling + lots and lots of support from friends and family led me back to race running – this is the 10k Blue Bell fun run in Brenham, TX. Please don’t give up. Get a good Ortho and good PT (if there is anyone out there in Houston, I have recommendations for both after suffering through several bad experiences). I have been running 7 miles every Saturday with my buddies, riding horses again, and sitting through Broadway plays and movies with the help of a special pillow. I am not 100%, but at least 90% healed. Hang in there, I am cheering for all of you! (especially Vicki)

Sam’s Story
Almost 5 years ago I started to develop HHT. It started appearing while running, during a football pre-season. A sort of tugging feeling. I’ve never had a muscle/tendon injury before so I just assumed I’d run through it and it would get better.
It slowly got worse through tennis and football and before I knew it, I could barely kick off my shoe.
Over the next two years, I went to two chiropractors, one physio, one sports doctor and a deep tissue massage therapist.
Nothing seemed to work.
I just thought it would get better but I would always do something to hurt it …… like running or kicking without warming up etc.
The annoying thing about my injury, was if you did injure it further, you couldn’t feel the result until at least 1 – 2 days later.
I ended up going to another physio over a year ago. She recommended I started resistance training on my hamstrings and build up my glutes.
Slowly, I built up the strength in my hammy and was able to run at footy.
I had a lot of set-backs and had to restart again if I pushed it too hard running or kicking, if I didn’t warm up properly or did too much weight with exercises.
It’s been about a year now, I’ve been at 100% with sport. I still have to be smart and warm up but it’s good.
The key thing for me were:
Don’t do static stretches.
Do some dynamic stretches.
Glute and hamstring resistance training.
A good warm up before sport.
This is not an injury that can be fixed with rest. You must work at it using paced and graded exercises.
Most importantly, you gotta know your limits, don’t push too far because it might set you back.
Sam
Anonymous
I’d suffered with HHT for about 12 months (49 yrs old with a marathon / ultra marathon running background) and then thought I had gotten over it but had a really bad set back (after a 50km training run) that saw it flare up for another 4 months.
Have been 99% pain free for about 6 months now and have completed the Tokyo marathon and 2 x 100km trail races pain free during this time. Clams and more clams (daily) seemed to really help me along with continuing to load the tendon up to a tolerable point but being cautious not to over do it. I never really stopped running, but my speed definitely suffered.
By far the worst injury I’ve ever had, and I still feel like I’m not absolutely over it, despite how good the hammy feels. I’ve learned the pain signs that tell me when to back off, and also how important it is to keep exercising, keep running and avoid stretching and icing (at least for me). Good luck to everyone and definitely hang in, there is light at the end of a long tunnel.
Jason Liang Yihao’s Story
Hi all im about to share my road to recovery….
I have PHT 8 mths ago during a sprint and ever since my life changed totally.. i cant do my fav sports which is soccer as soccer would require the hammies all the time. I have done all the eccentrics exercises you name it i have done it and it is useless.
But today i am 90percent to my recovery already 10percent more to go to 100%How to i do it? Im going to share…
2 weeks ago i finally went for my 1st PRP injection (it is pain.. no joke).. after the 3rd day of the injection shockingly i felt the pain has worsen… i was devastated as i do not know what to do if this dont work. I called the clinic and then doc say usually the prp will take effect only on the 3 week n so i just carry on my daily schedule.
As the week progresses the pain became a dull ache instead of a sharp knife pain especially when perform long glute bridge exercise.
After the end of 2nd week of my PRP surprisingly one morning i woke up and find my usual stretch pain drop to 50%. NO JOKE 50%
The next 30% what i did was lots of eccentric exercises. The 2 exercises i felt the best was one legged squad and one legged long glute bridge. I did 3×15 and 3x20sec 2 times per day and it helps alot.
I have now return to running and going for my usual soccer soon. Update you guys again as i might consider going for the 2nd prp shot to solidify the PHT. As soccer playing needs 100%
Good luck guys… Trust me PRP+ eccentric so far has helped me.
You may PM me if you need any help i can share with you more.
Thank you and good luck guys
Anonymous
One year ago I injured my hamstring on a short run, trying to increase speed by raising my feet up more. During a long run a couple of days later, I experienced sharp, constant pain in my left glute. I regularly see a chiropractor, who felt it was normal soreness that I could work through. In the meantime, it was painful to sit – any length of time in a chair hurt and cramped my whole thigh. Toilet seats were really rough, as the defined seat seemed to put sharp pressure right against the sorest area, around my left sit-bone.
I knew in my heart this wasn’t something I could just work though and scheduled with a sports-specific PT that had been recommended to me by another athlete. I was diagnosed with high hamstring tendinopathy or PHT. My running got cut back drastically and I had two PT appointments a week to start. These consisted of very small weird movements to address WHY I’d gotten PHT, which was one legs’ dominance, some weaker support muscles, and a hip imbalance. I also got a balance disk to sit on at work which helps keep some pressure off the sit-bone.
I was discharged from PT after six months and was back at half marathon distance without pain. I have PT exercises to do before every run, and my PT person taught me how to detect my imbalance and which exercises I could keep doing from my six months in PT to help address it. One year later, I might feel an occasional brief ache in that area from either sitting too much or after a long run, but it’s fleeting. I have PT exercises I will have to do forever if I want to keep it that way, but it’s worth it.
I wish everyone with PHT the best in their healing, and hope you are able to fully recover.
Christine Bridges Back To Running!
Christine’s Recovery
I set out for a run with my running club in September 2018 and within a few minutes I had pain in both buttocks. I carried on run walking but it didn’t ease and I felt very stiff. The pain eased after a few days but I booked in with a physio and she said it sounded like sciatica or piriformis but was unusual as it was both sides in the centre of both bum cheeks. Anyway it seemed ok so I carried on running without any problem but one evening in November I tripped over a manhole cover whilst running. I didn’t fall but stumbled taking me some time to recover and I carried on running back to club. The next day I could barely walk, the pain in my bum was much worse and I couldn’t bend down with bent knees. Again I went to physio but this time a friend of mine (she lives 2 hours away from me) and she was doubtful it was piriformis or sciatica but she gave me a good massage and it seemed a lot better.
Anyway I think at this point I should have told my stubborn self to go to the doctors, but I didn’t. I did a race in December it was going to be 10k but I opted for the 5k. It was bitterly cold and boring and when I finished I could hardly move, my friend wondered what was wrong with me and I thought I was just stiffening up with old age!
Needless to say I carried on running into 2019 and was seeing another physio who thought it was piriformis but odd as it was both sides. In May I drove my friends to a Parkrun an hour away and when I got home I couldn’t get out of the car. I decided then I had to go to my GP, enough was enough. I stopped running.
I was sent for an MRI scan on my spine and referred to a consultant. He said although he could see I had wear and tear on my lower spine this was to be expected at my age, 66, but wasn’t the cause of my pain. He sent me the next day for another MRI on my hips and with this he gave me the diagnosis of Proximel Hamstring Tendinothapy it was the end of July this year. I was referred for physio at the local hospital. Her advice was to do a few stretching exercises and some strengthening exercises. After a couple of weeks she did ultrasound actually on my bum and I could barely walk the next day. Not very helpful.
The problem I also had was that I was going to the USA at the end of September so I needed to endure a 9 hour flight plus a 4 hour drive at the other end. The physio advised that I go for the steroid injections offered by my consultant so I made an appointment. The hospital was 2 hours away and when I got there the consultant, a different one, could not do the injections because he had no scanner to guide him. He advised that I go home a take a course of ibuprofen. No other professional had advised me to take these. I was not happy that I’d driven all that way to be told this but determined to prove him wrong, I took the ibuprofen.
Well after a few days the pain on bending and sitting had eased a bit. I was offered another appointment for the injections one day before my flight and I refused this and carried on taking the ibuprofen. Amazing! That’s all I can say and I know this would not work for everyone but it was total revelation to me! I bought a travel seat cushion for the flight and I had no pain or stiffness at all and I carried on taking the ibuprofen. I thoroughly enjoyed my visit to my son in the USA.
In total I took it for 6 weeks, each time with food and then I started with strengthening exercises. Reducing the ibuprofen too. In November I joined the local gym and signed up with the Personal Trainer who has given me some valuable advice about my running gait and also a strengthening program. I also found a good sports massage guy who has also given me good advice. I started Couch to 5k and I’m now on week 5 and running for 8 minutes!
I have the odd twinge but I can drive for two hours, sit ok and bend to the floor with legs bent. It’s been hard work and I’m taking things very very steady as I don’t want to undo my hard work. I certainly feel much stronger and more toned and will be running back with my club again soon, although not in the dark! I hope this gives hope to those still suffering. X 😊
To talk to people who have recovered, visit the PHT Facebook page:
https://www.facebook.com/ProximalHamstringTendinopathy







 Stuart Butler
Stuart Butler


 Hannah Erl – Marathon Runner Tells Her Emotional Story of PHT and Surgery by Dr. Lasse Lempainen
Hannah Erl – Marathon Runner Tells Her Emotional Story of PHT and Surgery by Dr. Lasse Lempainen

